Your new post is loading...
 Your new post is loading...

|
Scooped by
nrip
|
The recent SARS-CoV-2 pandemic underscored the effectiveness and rapid deployment of digital public health interventions, notably the digital proximity tracing apps, leveraging Bluetooth capabilities to trace and notify users about potential infection exposures. Digital proximity tracings showcased the promise of digital public health. As the world pivots from pandemic responses, it becomes imperative to address noncommunicable diseases (NCDs) that account for a vast majority of health care expenses and premature disability-adjusted life years lost. The narrative of digital transformation in the realm of NCD public health is distinct from infectious diseases. The power of artificial intelligence (AI) in this digital transformation is noteworthy. - AI can automate repetitive tasks, facilitating health care providers to prioritize personal interactions, especially those that cannot be digitalized like emotional support.
- Moreover, AI presents tools for individuals to be proactive in their health management. However, the human touch remains irreplaceable;
- AI serves as a companion guiding through the health care landscape.
Digital evolution, while revolutionary, poses its own set of challenges. Issues of equity and access are at the forefront. Vulnerable populations, whether due to economic constraints, geographical barriers, or digital illiteracy, face the threat of being marginalized further. This transformation mandates an inclusive strategy, focusing on not amplifying existing health disparities but eliminating them. Population-level digital interventions in NCD prevention demand societal agreement. Policies, like smoking bans or sugar taxes, though effective, might affect those not directly benefiting. Hence, all involved parties, from policy makers to the public, should have a balanced perspective on the advantages, risks, and expenses of these digital shifts. For a successful digital shift in public health, especially concerning NCDs, AI’s potential to enhance efficiency, effectiveness, user experience, and equity—the “quadruple aim”—is undeniable. However, it is vital that AI-driven initiatives in public health domains remain purposeful, offering improvements without compromising other objectives. The broader success of digital public health hinges on transparent benchmarks and criteria, ensuring maximum benefits without sidelining minorities or vulnerable groups. Especially in population-centric decisions, like resource allocation, AI’s ability to avoid bias is paramount. Therefore, the continuous involvement of stakeholders, including patients and minority groups, remains pivotal in the progression of AI-integrated digital public health. read the original paper at https://publichealth.jmir.org/2024/1/e49575/

|
Scooped by
nrip
|
The aim of the Connected Healthcare Study was to understand the impact COVID-19 has had on health care and communication with providers and gain insights into experiences and preferences as it relates to telehealth and online health care tools. More than two-thirds of U.S. patients (69%) had seen a health care provider via telehealth since the COVID-19 pandemic began, with more than two in five (46%) meeting with a PCP and about one in five (19%) meeting with a mental health care provider. Other providers whom respondents have seen via telehealth since the pandemic began included specialties like ophthalmology and women’s health and orthopedic care, which were not considered typical telehealth users before the pandemic. Telehealth is clearly emerging from the COVID-19 pandemic as the new normal – an overwhelming majority (84%) of respondents who received telehealth services since March 2020 reported that they plan to continue using telehealth appointments in the future, with the top reasons being that it’s more convenient (43%) or to avoid being around people who are ill (39%). One of the most striking results of the survey was that nearly half of U.S. patients (48%) reported that they have sought (4%) or would be likely to seek care (44%) from a different health care provider if their current provider did not offer telehealth appointments. This is clearly a resounding message of support for telehealth from patients to their physicians. As we look back on the broader impact of the COVID-19 pandemic, it will have catapulted patient awareness and acceptance of telehealth and virtual care to the extent that would have been inconceivable before the pandemic. It has also brought to the forefront many other aspects of patient electronic and virtual engagement with providers across all specialties. read the entire post at https://www.kevinmd.com/blog/2021/05/how-do-patients-really-feel-about-virtual-care-and-electronic-patient-engagement.html

|
Scooped by
nrip
|
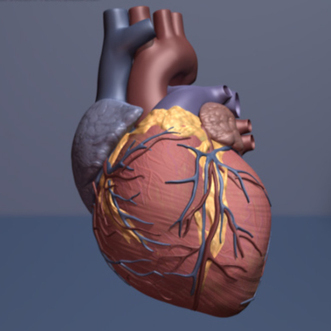
In recent times, researchers have increasing found that the power of computers and artificial intelligence is enabling more accurate diagnosis of a patient's current heart health and can provide an accurate projection of future heart health, potential treatments and disease prevention In a paper published in the European Heart Journal, researchers from King's College London, show how linking computer and statistical models can improve clinical decisions relating to the heart. The research team is lead by Dr. Pablo Lamata. In his statement he said that "We found that making appropriate clinical decisions is not only about data, but how to combine data with the knowledge that we have built up through years of research." The Digital Twin The team have coined the phrase the Digital Twin to describe this integration of the two models, a computerised version of our heart which represents human physiology and individual data. "The Digital Twin will shift treatment selection from being based on the state of the patient today to optimising the state of the patient tomorrow, The idea is that the electronic health record will be growing into a more detailed description of what we could call a digital avatar, a digital representation of how the heart is working. This could mean that a trip to the doctor's office could be a more digital experience. " Mechanistic models see researchers applying the laws of physics and maths to simulate how the heart will behave. Statistical models require researchers to look at past data to see how the heart will behave in similar conditions and infer how it will do it over time. Models can pinpoint the most valuable piece of diagnostic data and can also reliably infer biomarkers that cannot be directly measured or that require invasive procedures. "It's like the weather: understanding better how it works, helps us to predict it. And with the heart, models will also help us to predict how better or worse it will get if we interfere with it." read the original unedited article at https://medicalxpress.com/news/2020-03-digital-heart-future-health.html

|
Scooped by
nrip
|
Pokémon GO illuminated the potential for mobile phone gaming apps to engage users and promote health. However, much work is needed to fully understand the mechanisms through which digitally supported behavior change interventions operate, particularly for children and families. Objective: The aims of this study were (1) to explore the Pokémon GO user experience from a family perspective and (2) to investigate Pokémon GO within the context of family health. Methods: Between January and February 2017, congruent with one of the largest anticipated Pokémon GO updates Gen 2, participants were recruited from parks, word of mouth, and social media to complete a Web-based survey. Participants were surveyed about family characteristics, interest, and experiences playing Pokémon GO and healthy lifestyle beliefs. Using a revised Godin Leisure-Time Exercise Questionnaire, a retrospective pre-post design assessed changes in parent physical activity (PA) before and after playing Pokémon GO. Pokémon GO transcended traditional understanding of digital health and uniquely reached across generations to engage users. Findings from this study highlight that, for a period of time, Pokémon GO fostered social and physical well-being for children and families through a multifaceted approach. read the study at https://pediatrics.jmir.org/2018/2/e10679/

|
Scooped by
nrip
|
Doctors are using digital tools and willing to receive data feeds from their customers, but they are quite frustrated by poor usability of digital healthcare tools and difficulty getting measurable results
Common Complaints:
• EHRs are typically hard to use. Many doctors I know complain of spending several extra hours each day entering data to EHRs. In some practices medical scribes have been added to help with data entry.
• EHRs are often local, island systems that do not provide access to other clinical resources, so doctors need to use multiple systems.
• Patient portals are often a dismal experience. HIPAA has motivated administrators to mandate defensive designs that are often so inconvenient for patients that they are seldom used, which I suppose makes them highly secure.
• Doctors feel they have tons of data available to them, but few tools to use it to make intelligent and timely decisions.

|
Scooped by
nrip
|
A recent international survey by the McKinsey & Company consulting firm addresses some myths about consumer use of digital healthcare services.
Many healthcare executives believe that, due to the sensitive nature of medical care, patients don’t want to use digital services except in a few specific situations. Decision makers often cite relatively low usage of digital healthcare services. Results of this survey however reveal something quite different.
The 5 myths debunked by this survey are as follows Myth 1: People don’t want to use digital services for healthcareMyth 2: Only young people want to use digital services Myth 3: Mobile health is the game changerMyth 4: Patients want innovative features and appsMyth 5: A comprehensive platform of service offerings is a prerequisite for creating value
More at http://www.healthdatamanagement.com/gallery/5-myths-about-consumer-use-of-digital-healthcare-services-48388-1.html

|
Scooped by
nrip
|
The most accurate simulation of the human brain to date has been carried out in a Japanese supercomputer, with a single second’s worth of activity from just one per cent of the complex organ taking one of the world’s most powerful supercomputers 40 minutes to calculate.
Researchers used the K computer in Japan, currently the fourth most powerful in the world, to simulate human brain activity. The computer has 705,024 processor cores and 1.4 million GB of RAM, but still took 40 minutes to crunch the data for just one second of brain activity.
The project, a joint enterprise between Japanese research group RIKEN, the Okinawa Institute of Science and Technology Graduate University and Forschungszentrum Jülich, an interdisciplinary research center based in Germany, was the largest neuronal network simulation to date. It used the open-source Neural Simulation Technology (NEST) tool to replicate a network consisting of 1.73 billion nerve cells connected by 10.4 trillion synapses.
While significant in size, the simulated network represented just one per cent of the neuronal network in the human brain. Rather than providing new insight into the organ the project’s main goal was to test the limits of simulation technology and the capabilities of the K computer.

|
Scooped by
nrip
|
A list of healthcare and digital health influencers to follow in 2014.

|
Scooped by
nrip
|
You CAN step into the realm of digital health and stay on the right side of the law This is an Introduction to Digital Health presented at the Massachusetts Bar Association "Hot Topics in Healthcare" program on December 10, 2013 by David Harlow. For more information, see related posts at HealthBlawg.com.
|

|
Scooped by
nrip
|
We discuss the concept of a participatory digital contact notification approach to assist tracing of contacts who are exposed to confirmed cases of coronavirus disease (COVID-19); The core functionality of our concept is to provide a usable, labor-saving tool for contact tracing by confirmed cases themselves the approach is simple and affordable for countries with limited access to health care resources and advanced technology. The proposed tool serves as a supplemental contract tracing approach to counteract the shortage of health care staff while providing privacy protection for both cases and contacts. - This tool can be deployed on the internet or as a plugin for a smartphone app.
- Confirmed cases with COVID-19 can use this tool to provide contact information (either email addresses or mobile phone numbers) of close contacts.
- The system will then automatically send a message to the contacts informing them of their contact status, what this status means, the actions that should follow (eg, self-quarantine, respiratory hygiene/cough etiquette), and advice for receiving early care if they develop symptoms.
- The name of the sender of the notification message by email or mobile phone can be anonymous or not.
- The message received by the contact contains no disease information but contains a security code for the contact to log on the platform to retrieve the information.
Conclusion The successful application of this tool relies heavily on public social responsibility and credibility, and it remains to be seen if the public would adopt such a tool and what mechanisms are required to prevent misuse. This is a simple tool that does not require complicated computer techniques despite strict user privacy protection design with respect to countries and regions. Additionally, this tool can help avoid coercive surveillance, facilitate the allocation of health resources, and prioritize clinical service for patients with COVID-19. Information obtained from the platform can also increase our understanding of the epidemiology of COVID-19. read this concept paper at https://mhealth.jmir.org/2020/6/e20369

|
Scooped by
nrip
|
The American Health Information Management Association is giving providers a resource site for evaluating digital health tools, and giving mHealth vendors an opportunity to seek AHIMA certification. AHIMA has unveiled AHIMA dHealth, a site which offers resources for healthcare providers on digital health products, including privacy and data security practices and policies, and an assessment tool designed to help vendors meet AHIMA standards. To become AHIMA-certified, a vendor will have to complete a self-reported assessment based on the organization’s standards and best practices for privacy and security. As per the CEO of AHIMA, “Earning AHIMA dHealth Approval shows that your product takes privacy and data security seriously, Having this designation allows developers to build trust with providers and patients, which has the potential to earn and positively impact more users.” CVS Health is also giving the digital health industry some love. The company has launched a $100 million venture capital fund targeting early-stage companies that are developing “cutting-edge, digitally enabled solutions.” to learn more read the entire article at https://mhealthintelligence.com/news/ahima-launches-mhealth-resource-assessment-tool-for-vendors

|
Scooped by
nrip
|
We are directionally headed towards a significant shift in the way care is delivered. The rapid up scaling of virtual care capacity and the mainstreaming of Telehealth have given rise to new digital health tools. Self-triaging and contact tracing for COVID-19 infection detection are among the new breed of digital health applications that startups to big firms alike were looking at to seize the emerging opportunities. Telehealth is here to stay. Healthcare is shifting to virtual care models. Digital front door apps are all the rage. What else is emerging that could change the way we experience care? While telehealth is now the de facto mode of accessing healthcare for most low-acuity and routine care needs, a number of related technology-led trends are quietly gaining ground as well. Here the author looks at a few of these and opinionates on their potential impact on healthcare consumer experiences. "contactless" experiences: Covid has made us all afraid to touch any surface exposed to the public. Nowhere is this fear more prominent than a hospital or clinic setting. Healthcare executives now speak of airport check-in type of experiences for healthcare appointments, both for in-person and virtual visits. Technology-enabled workflows now enable patients to complete most of the registration formalities prior to the visit, be it a virtual consult or a clinic visit. Registration kiosks in hospital lobbies may soon be enabled with facial recognition software to eliminate the need for touching any surface. Routine examinations are also going virtual, with many diagnostic procedures now possible through remotely controlled devices. Caregivers are beginning to do their patient rounds through virtual visits. This trend will only grow in the coming years. Contact tracing Inspired by the success of India, Singapore and South Korea, contact tracing applications on Bluetooth-enabled devices have been positioned as an effective means to track and trace infections to reduce the spread of COVID-19 Despite many setbacks, contact tracing's potential for deployment within communities and populations for uses beyond COVID-19 has longer-term potential, and this could be the single most important technology-enabled healthcare program to come out of the COVID-19 crisis. Remote monitoring and automated communication Healthcare executives are more motivated than ever to keep their populations healthy in their homes. A vast and growing array of automated communication tools allows caregivers to use rule-based messaging to push everything from health coaching, post-discharge care instructions, and appointment reminders through IVR, text, SMS, and mobile alerts. Data mining tools can identify subsets of populations at risk and enable caregivers to intervene on time. A New York-based COVID-19 Rapid Response Coalition involving tech giant Amazon that targeted high-risk populations through SMS campaigns that reached up to 10,000 members a day, is an example of how automated communication tools can serve populations in a crisis and during normal times. The use of digital health and automated communication tools has also improved healthcare outcomes by reducing no-shows for appointments, increased adherence to medication regimens, and targeted interventions during adverse events. There is an unprecedented opportunity today to use telehealth technologies in the complete continuum of care. However, healthcare enterprises and their technology partners need to make them more user-friendly. That will determine success for new technology-enabled virtual care models. Every health system has to design the digital experience that is suited for their patient populations while remembering to address the needs of caregivers who will deliver and manage the experiences.

|
Scooped by
nrip
|
Every day, around the world, an estimated 830 women die from pregnancy or childbirth related causes, most in low-income countries. An additional 7000 newborn babies die each day. Many of these deaths could have been prevented. The presence of a skilled birth attendant—doctor, nurse, or midwife—at birth is important to prevent and manage obstetric complications. Supportive care from birth companions can also be helpful to women by bringing support, monitoring, and care to a woman's home throughout pregnancy, labour, and post partum. Imagine if a digital toolkit could be given to pregnant women that combines the ability to individually support, monitor, and inform them, but does it remotely using sensors and apps. It could also incorporate artificial intelligence algorithms to identify patterns of high-risk complications before they occur and could potentially prevent them.

|
Scooped by
nrip
|
A team of researchers out of Duke University recently announced they’ve grown human skeletal muscle in a dish. The muscle responds to electrical impulses, biochemical signals, and drugs just like muscle tissue in our bodies. It’s hoped that in the future such lab-grown tissues might serve as a way to test new drugs and study diseases outside the human body without risking a patient’s health. They might also be used to provide more personalized therapies.
“We can take a biopsy from each patient, grow many new muscles to use as test samples and experiment to see which drugs would work best for each person,” said Nenad Bursac, associate professor of biomedical engineering at Duke and a lead researcher on the study. Bursac and Lauran Madden, a postdoctoral researcher in Bursac’s laboratory, grew the muscle tissue by first adding “myogenic precursors,” a kind of proto muscle cell, to a three-dimensional scaffolding and nutrient gel in a dish. As the cells matured, they lined up and formed working muscle fibers (shown here at the top of the page).

|
Scooped by
nrip
|
So far the internet of things hasn’t made much headway into patient care in the medical setting, but consumers are buying wellness devices for a variety of reasons. Will the medical world embrace that data?
The intersection of healthcare and connected devices was thrown into high relief these last few weeks as both Apple and Samsung unveiled ecosystems to take consumer health data and turn it into actionable intelligence.
But this week’s guests at the Weekly podacst at GigaOm are confident that as advanced as consumer-grade consumer grade health devices get, they won’t become something doctors are hot on for years to come — if ever.
In this week’s podcast Stacey Higginbotham discusses medical connected devices and where it may meet the consumer with Rick Valencia from Qualcomm Life. Will doctor’s prescribe our apps or devices?

|
Scooped by
nrip
|
A credit card-sized chip can diagnose HIV infection and provide T cell counts to guide treatment, according to a recent paper in Science Translational Medicine.
The fluid-processing chip provides accurate test results in less than 20 minutes using a single drop of blood that goes directly into the testing chamber and does not require trained handling.
The chip is designed to work in a battery-powered handheld device that would “deliver simple HIV diagnostics to patients anywhere in the world, regardless of geography or socioeconomic status,” the researchers say in the paper.
Nearly 7 in 10 HIV-infected people live in poor parts of the world. Many have to travel long distances to get to a clinic, making coming back for test results a major ordeal.
#1. Isolation & Loss of Human Touch Yes, patients need technology and progressive medical devices to manage their health. But they also need to be seen, listened to, and cared for (physically) by other people, including doctors, nurses and caregivers. Empathy and compassion – a warm smile, a kind word, or a re-assuring tone are equally important in bringing about health and wellness.
I worry that too much focus on digital healthcare, (and conversely too few in-person experiences between doctors and patients) might lead to feelings of isolation, remoteness and even doubt.
Patients who are more passive in nature may even resist the shift to greater personal responsibility and technology-based guidance. The result: They end up feeling like they don’t really have any support to manage their health.
#2. Marginalization of the Poor While we can all agree that significant advantages are being realized through ehealth products and services, we also have to admit that these technologies mostly benefit those who have access to greater resources.
In fact a 2007 study published in the U.S. National Library of Medicine warned that significant challenges must be addressed by the research community to assure that advances in e-health will help eliminate, not intensify health disparities.
I know it’s hard to believe, but there are many people in this country who don’t have access to the Internet, or even a home computer. How will e-health reach these people? The fact is, people or communities with limited access to digital technology are largely the same as those suffering the greatest health disparities and traditionally underserved by the healthcare system.
#3. Information overload Today, patients are more empowered. They have access to information that can help them make better decisions about their health – in an ideal world.
But as the volume of personal health and wellness data from medical devices, smartphone apps, and even EMR’s increases, patients will be faced with information overload and some may find it hard to act upon.
For passive patients in particular, having too much information at their disposal might actually lead to inaction rather than action, because they’re used to simply following doctor’s orders. In addition to being sick they now have the added burden of figuring out what their health data means and what to do about it.
What do you think?
Read more: http://wordviewediting.com/3-unintended-consequences-of-digital-health/
Via Parag Vora

|
Scooped by
nrip
|
A new interdisciplinary research center at MIT, funded by the National Science Foundation, aims at nothing less than unraveling the mystery of intelligence.
The new center headquartered at the Massachusetts Institute of Technology will focus on bringing researchers from separate fields together to try and crack one of the biggest questions facing science today: what is intelligence, and how can we engineer it?
By tapping a broad range of expertise, including scholars who study how a baby’s mind develops and others trying to understand how the brain makes sense of social situations, the researchers hope to take a definitive step forward over the next five years toward the long-held goal of understanding intelligence and building computers capable of thinking like people.
The center’s four main research themes are also intrinsically interdisciplinary. They are the integration of intelligence, including vision, language and motor skills; circuits for intelligence, which will span research in neurobiology and electrical engineering; the development of intelligence in children; and social intelligence. Poggio will also lead the development of a theoretical platform intended to undergird the work in all four areas.
“Those four thrusts really do fit together, in the sense that they cover what we think are the biggest challenges facing us when we try to develop a computational understanding of what intelligence is all about,” says Patrick Winston, the Ford Foundation Professor of Engineering at MIT and research coordinator for CBMM.
For instance, he explains, in human cognition, vision, language and motor skills are inextricably linked, even though they’ve been treated as separate problems in most recent AI research. One of Winston’s favorite examples is that of image labeling: A human subject will identify an image of a man holding a glass to his lips as that of a man drinking. If the man is holding the glass a few inches further forward, it’s an instance of a different activity — toasting. But a human will also identify an image of a cat turning its head up to catch a few drops of water from a faucet as an instance of drinking. “You have to be thinking about what you see there as a story,” Winston says. “They get the same label because it’s the same story, not because it looks the same.”
Sources:
http://web.mit.edu/newsoffice/2013/center-for-brains-minds-and-machines-0909.html
http://www.boston.com/news/science/blogs/science-in-mind/2013/09/09/mit-center-receives-million-unravel-the-mysteries-human-intelligence/SKNU4umjtPy5pN7nFnYcXL/blog.html
|



 Your new post is loading...
Your new post is loading...